Symptomatic paroxysmal atrial fibrillation in a patient with unilateral pulmonary vein atresia
Keywords:
Atrial fibrillation, pulmonary vein atresia
Abstract
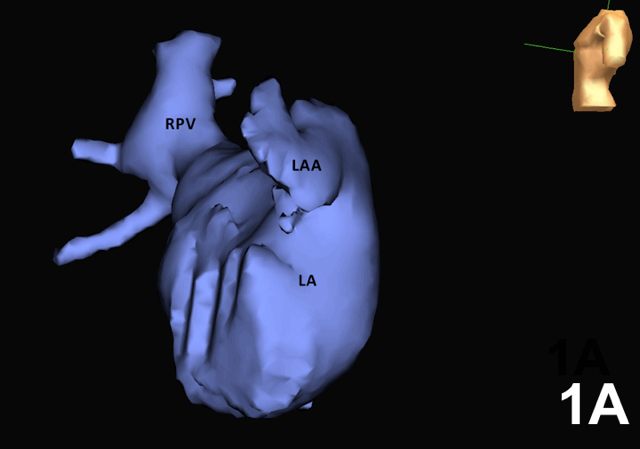
A 52-year-old man with symptomatic paroxysmal atrial fibrillation was offered an atrial fibrillation (AF) ablation procedure. His echocardiogram indicated that he had no structural heart disease. A cardiac computed tomographic (CT) scan showed enlargement of the right pulmonary veins, absence of the left pulmonary veins, a prominent left atrial appendage, and a hypoplastic left lung. Cardiac CT with an electroanatomic mapping system confirmed a prominent left atrial appendage and the absence of the left pulmonary veins. Due to the limited number of patients with this condition, information about ablation remains very limited, and his ablation was deferred. Unilateral pulmonary vein atresia is a rare condition in adults which results from failure of incorporation of the common pulmonary vein into the left atrium. This case demonstrates the clinical importance of preprocedural imaging prior to AF ablation.Downloads
Download data is not yet available.
Published
2015-01-04
How to Cite
Sehli, S., & Donaldson, D. M. (2015). Symptomatic paroxysmal atrial fibrillation in a patient with unilateral pulmonary vein atresia. The Southwest Journal of Medicine, 3(9), 49-51. Retrieved from https://pulmonarychronicles.com/index.php/pulmonarychronicles/article/view/182
Section
Case Reports




