An unusual mycobacterial infection
Abstract
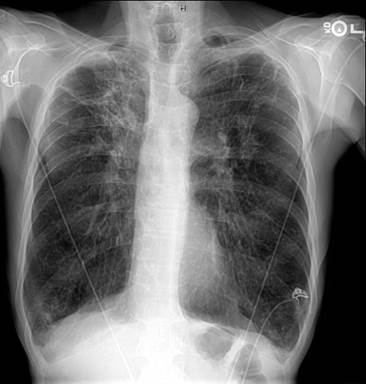
The frequency of atypical mycobacterial or nontuberculous mycobacterial (NTM) infections has increased during the last three decades with the emergence of HIV/AIDS and more use of immunosuppressive treatments. We present a case of pulmonary mycobacterial infection secondary to Mycobacterium kansasii in a patient with chronic obstructive pulmonary disease (COPD) and malnutrition. M. kansasii is a ubiquitous organism, most commonly found in the southern and central regions of the US. It can occur as a colonizer, but when it produces disease it usually involves the lung. The American Thoracic Society (ATS) and Infectious Diseases Society of America (IDSA) have issued criteria to differentiate casual NTM isolation from true pulmonary NTM disease. Among the NTM infections, M. Kansasii is the pathogen which causes a clinical picture which most resembles pulmonary tuberculosis. It can produce a bronchiectasis, nodular lesions, and/or fibrocavitary infiltrates on x-rays. Treatment requires a rifampin based regimen, usually combined with isoniazid and ethambutol. If rifampin resistance is present, macrolides, quinolones, or sulfas are usually recommended.
Downloads